AbstractBackgroundPupillary light reflex (PLR) assessment is an important neurological examination reflecting neurological deterioration in severe stroke cases. This study investigated the impact of diurnal variation in the PLR using quantitative pupillometry in stable patients with large hemispheric stroke.
MethodsWe included 35 patients with large hemispheric stroke without neurological worsening, who were admitted to the neurological intensive care unit between April 2017 and November 2021. Quantitative pupillometry was performed every 4 hours. Pupillometer parameters of maximum pupil size, percentage of constriction (%CH), latency (LAT), constriction velocity (CV), dilation velocity (DV), maximum constriction velocity (MCV), and neurological pupil index (NPi) score were recorded. We evaluated changes in the pupillometer parameters over time using linear mixed model analysis.
ResultsThe diurnal variations revealed that the following parameters were significantly higher at 04:00 than at 20:00: maximum pupil size (right [Rt]: 3.59 vs. 3.21 mm, P<0.001; left [Lt]: 3.51 vs. 3.18 mm, P<0.001), %CH (Rt: 31.48 vs. 25.72, P<0.001; Lt: 31.42 vs. 24.98, P<0.001), CV (Rt: 1.97 vs. 1.68 mm/sec, P<0.001; Lt: 1.98 vs. 1.65 mm/sec, P<0.001), and DV (Rt: 0.97 vs. 0.84 mm/sec, P<0.001; Lt: 0.94 vs. 0.82 mm/sec, P=0.001). However, no significant diurnal variations were observed in the NPi values.
INTRODUCTIONPupillary light reflex (PLR) assessment is a crucial neurological examination in neurologically critical patients. A quantitative pupillometer allows quantitative and objective assessment of the PLR. Therefore, it is widely accepted as a reliable and standard tool for assessing the PLR during neurological examination in the neurological intensive care unit (neuroICU) [1-4]. An acute change in the PLR based on the pupillometer is an early indicator of increased intracranial pressure (ICP) or worsening intracranial pathology. Additionally, significant deterioration in the pupillometer parameters, including the neurological pupil index (NPi), has been linked to worsening ICP or midline shift [5-7].
Pupillary reactivity, including pupil size, is influenced by the sleep cycle, circadian rhythm, changes in autonomic nervous system status, and ambient light levels, which could show diurnal variations [8-13]. Therefore, changes in the PLR or pupil size could be due to the time-of-day effect. However, the extent of the effects of the diurnal factors on the interpretation of PLR remains unclear in patients with large stroke in the neuroICU. The time-of-day effect has rarely been considered on the PLR based on the pupillometer parameters assessed over 24 hours in patients with large hemispheric stroke and stable neurological symptoms. Therefore, this study aimed to investigate the variations in pupillometer parameters at different time points over 24 hours in large hemispheric stroke patients without neurological deterioration.
METHODSStudy populationThis retrospective study initially screened 65 patients, who were admitted to the neuroICU between April 2017 and November 2021 for large hemispheric stroke (ischemic or hemorrhagic) and were evaluated using a pupillometer. The exclusion criteria were as follows: (1) neurological worsening during monitoring (n=18), (2) posterior circulation stroke (n=5), and (3) missing values in the serial PLR data (n=7), depending on the neurological condition and time interval of neurological assessment. Finally, 35 patients with anterior circulation stroke were included in the analyses and evaluated using an automated pupillometer during monitoring.
Baseline characteristics and clinical informationWe analyzed the clinical information and demographic variables, including age, sex, and vascular risk factors such as hypertension, diabetes mellitus, dyslipidemia, coronary artery disease, atrial fibrillation, history of stroke, and pre-stroke functional status. The patients’ diagnoses and lesion sites were assessed during admission. Neurological severity was evaluated using the Glasgow Coma Scale (GCS) at admission and every 4 hours during monitoring. Moreover, information regarding sedation therapy was collected during the monitoring period.
Measurement of quantitative pupillary reactivityWhen the neurological symptoms were stable, quantitative pupil assessment was performed using NPi-100 Pupillometer (NeurOptics Inc.) every 4 hours by neurointensivists or neuroICU nurses in charge of the standard care of patients. The pupillometer parameters of maximum pupil size, percentage of constriction (%CH), constriction velocity (CV), maximum constriction velocity (MCV), dilation velocity (DV), latency (LAT), and NPi in the right and left eyes were recorded at 0:00, 4:00, 8:00, 12:00, 16:00, and 20:00 [1,2,4]. The values recorded at 20:00 were considered as the baseline, as the lights were turned off at 00:30 in the neuroICU. The pupillometer parameters were then paired with the GCS scores at each time point.
Statistical analysisBaseline characteristics and clinical information were used for descriptive analysis. Nominal data are presented as frequencies (%), normally distributed continuous variables as means±standard deviations, and non-normally distributed continuous variables as medians and interquartile ranges (IQRs). We compared the pupillometer parameters according to the lesion side of the stroke (ipsilateral side or contralateral side). Additionally, the change in the pupillometer parameters at different times during monitoring was analyzed using a linear mixed model with a random intercept model for repeated measures analysis, adjusting the GCS score at each time point of pupillary reactivity measurement as the fixed factor. Statistical significance was set at P-value <0.05. All statistical analyses were conducted using IBM SPSS ver. 25.0 (IBM Corp.), Statistical Analysis Software 9.4 (SAS Institute Inc.), and GraphPad Prism (version 9, GraphPad Software).
RESULTSAmong the 35 included patients (mean age, 69.5 years; 62.9% men), 951 measurements of quantitative bilateral pupillary assessment were performed and analyzed. The baseline characteristics and clinical information are described in Table 1. Regarding diagnosis, 62.9% (n=22) of the patients had ischemic stroke, and the rest had hemorrhagic stroke. The median initial GCS score at admission was 10 (IQR, 9–12). Functional independence before the index stroke was observed in 60.0% of the patients (modified Rankin Scale score=0) (Table 1).
For the automated pupillometer parameters, the median number of pupillary measurements was 25 (IQR, 14–26) during the monitoring period. When comparing the pupillometer parameters between the lesion and contralateral sides, none of the parameters differed significantly, except the maximum pupil size. The maximum pupil size was significantly larger on the contralateral side than on the ipsilateral side at all times, although the difference was within 0.3 mm (Table 2). Table 3 shows the pupillometer variables over 24 hours. Regarding the maximum pupil size, the baseline pupil size at 20:00 did not differ between the right and left pupils. At all monitoring times over 24 hours, the change in the maximum pupil size showed a significant diurnal variation (P for linear trend; right [Rt]: P<0.001, left [Lt]: P=0.001). The maximum pupil size bilaterally was significantly larger at 0:00 and 4:00 (Rt: 3.56±1.09 mm and 3.59±1.03 mm; Lt: 3.40±1.10 mm and 3.51±1.02 mm, respectively) than at 20:00 (Rt: 3.21±0.93 mm; Lt: 3.18±0.89 mm) (Table 3, Fig. 1). The baseline %CH values were similar in the bilateral pupils. As observed in the maximum pupil size, the %CH values were higher at 0:00 and 4:00 (Rt: 27.48±10.00 and 31.48±8.65; Lt: 27.56±10.51 and 31.42±9.45, respectively) than at 20:00 (Rt: 25.72±9.86, Lt: 24.98±10.45), with a significant diurnal variation observed (P for linear trend; Rt: P<0.001, Lt: P<0.001) (Table 3, Fig. 1). The LAT did not differ at any time point, regardless of the side. No significant differences in the baseline bilateral CV and MCV were observed at 20:00. The CV and MCV at 0:00 and 4:00 were significantly higher than the baseline values at 20:00, whereas those during the daytime did not change significantly. There were significant diurnal variations in the CV (P for linear trend; Rt: P<0.001, Lt: P=0.001) and MCV (P for linear trend; Rt: P<0.001, Lt: P<0.001) over 24 hours (Table 3, Fig. 1). The DV at baseline did not differ significantly between the right and left sides. Moreover, it showed a similar time trend as observed for the aforementioned parameters. The DV at 0:00 and 4:00 was higher than that at 20:00, with a significant diurnal variation (P for linear trend; Rt: P=0.002, Lt: P=0.038) (Table 3, Fig. 1). The baseline NPi scores were similar on the right (4.36±0.46) and left (4.33±0.53) sides (P=0.564). No significant diurnal variations were observed in the right NPi score, although the left NPi score changed significantly over time; the left NPi score at 4:00 was higher than that at 20:00. Among the patients, five (14.3%) were administered dexmedetomidine during the monitoring period. We found that the trend of the PLR changes (largest pupil size at 04:00 and smallest size at 20:00) did not differ between the patients with and without dexmedetomidine treatment, suggesting that the dynamics of the pupillary variables were not affected by the use of dexmedetomidine (Supplementary Table 1).
DISCUSSIONThis study identified the time-of-day effect on pupillary parameters in large hemispheric stroke patients with stable neurological conditions. The maximum pupil size, %CH, CV, MCV, and DV were significantly higher during the night than during the day or evening; however, no sudden drop or significant change was identified in the pupillary parameters during the 24-hour monitoring.
Serial pupil examination is a basic but critical neurological examination performed in the neuroICU. In particular, quantitative assessment of the PLR using an automated pupillometer is a reliable and objective method for monitoring pupillary reactivity. Pupillometer assessment parameters, such as the NPi and CV, are reportedly sensitive to changes in neurological deterioration, which allows rapid diagnosis and evaluation of intracranial pathology and outcomes that assist in clinical decision-making following acute brain injuries [1-4,6,7,14-16]. Pupillometer parameters on the ipsilateral and contralateral sides were similar. However, the maximum pupil size was larger on the contralateral side than on the ipsilateral side. The maximum pupil size was within the normal range, and the observed difference between the contralateral and ipsilateral sides (less than 0.3 mm) was within the range of physiological anisocoria [17]. Changes in the PLR over 24 hours are influenced by lighting, circadian phase, balance in sympathetic and parasympathetic pathways, and sleepiness in everyday environments [13,18,19]. Previous studies investigating pupillary reactivity and pupil size over time have shown that pupil size increases at night, possibly due to alterations in the amount of light or changes in the circadian rhythm [8-10,19-21]. In contrast, other studies revealed that pupil size is dependent on the degree of sleepiness rather than the circadian phase [10,20,21]. Similarly, the relationship between pupillary dynamics and the time-of-day effect remains unclear, and no studies have investigated the diurnal variation in the pupillary parameters based on the pupillometer assessment of neurologically stable patients with large hemispheric stroke. This study revealed that pupil size was significantly larger at night, especially at 04:00, than during the day or evening (baseline value at 20:00), which corroborates the results of previous studies [8,9]. The pupillary parameters, including %CH, CV, MCV, and DV, gradually increased after 20:00; the highest values were recorded at 4:00 and the lowest at 20:00 over 24 hours, and these values could be associated with changes in pupil size. However, all pupillometer parameters had symmetric normative values with small oscillations over 24 hours.
Pupillary reactivity over 24 hours in large hemispheric stroke patients could be affected by modified circadian rhythms, light, and stimuli secondary to the environment in the neuroICU [18,19,22,23]. The circadian rhythm is affected by external stimuli, and critically ill patients commonly experience disrupted physiological circadian rhythms. Potential factors contributing to alterations in circadian rhythmicity in neuroICU patients include nocturnal light exposure, noise, altered feeding schedules, disease severity, scheduled nursing care, and sedative medications [22-24]. Therefore, pupil dynamics in the neuroICU may have been affected by the neuroICU environment influencing the patients’ circadian rhythms [18,19,22-25]. Additionally, pupil dynamics during the 24-hour cycle could be influenced by ambient light levels in the neuroICU. Ambient light levels in the neuroICU are usually controlled using artificial light with minimal sunlight impact [26]. Therefore, the schedule for turning lights on and off should be considered when interpreting the results. At our center, the lights were dimmed from 0:30 to 6:00 and switched on and maintained at the same level for the remaining time. The changes in the light level during the night might have affected the maximum pupil size and robust pupillary constriction response at 4:00. However, the trend of %CH showed an increase at 0:00 compared to the baseline value at 20:00 before the light level decreased, which suggests that the pupillary changes were not merely due to alterations in ambient light. Furthermore, the amount of sedative medication should be considered when interpreting changes in the PLR in the neuroICU [1,23]. In this study, the trends of the pupillometer parameters over time were similar in patients treated with and without sedative drugs.
This study has several limitations. First, this was a retrospective study with a small number of patients; therefore, an unmeasured bias may exist. Second, we did not evaluate the actual circadian rhythms in individual patients by assessing the melatonin levels. However, all patients were subjected to the same light and dark cycles in the same neuroICU environment. Third, we did not evaluate the intensity of ambient light in the neuroICU, which may have affected the pupillary reactivity. However, the light-on/light-off timings were regular and similar for all the patients. Therefore, the time-of-day effect related to light intensity on the changes in the PLR was similar for all included patients. Fourth, the level of consciousness and sedative drugs may have affected the PLR dynamics during the monitoring period. Therefore, we adjusted the GCS score at each time point for PLR monitoring using a linear mixed model analysis to minimize these effects. Moreover, treatment with sedation demonstrated similar time trends in the PLR of patients over 24 hours. Fifth, medical conditions and underlying diseases, such as retinopathy associated with diabetes mellitus, have the potential to affect the pupillometer parameters. Finally, the results were based on neurocritically ill patients who required repetitive pupillary assessments. Changes in pupillary dynamics may differ among healthy individuals. Additionally, most patients had a large hemispheric stroke, which may have affected the results. However, we do not think that the changes in pupillary values were merely due to alterations in neurological conditions because none of the patients experienced neurological worsening over the monitoring period, and the NPi scores did not deteriorate even with larger pupil sizes.
In conclusion, diurnal variations occurred in the pupillometer parameters over 24 hours in large hemispheric stroke patients who were in a stable neurological condition. However, all changes were within the normal ranges, with small oscillations. Therefore, transient changes in the PLR and physiological changes within normal ranges may be acceptable during neurological monitoring in neurologically critical patients. Additionally, serial monitoring of the PLR, regardless of the development of significant changes, could be a helpful tool for the neurological monitoring of large hemispheric stroke patients. Further large-scale studies are required to elucidate the relationship between the PLR parameters and time over 24 hours.
ARTICLE INFORMATIONEthics statement
This study was approved by the Institutional Review Board (IRB) of the Seoul National University Hospital (No. H-1009-062-332). The need for informed consent was waived by the IRB of Seoul National University Hospital because of the retrospective nature of the study. All methods were conducted in accordance with the relevant guidelines and regulations of the IRB of the Seoul National University Hospital.
Conflict of interest
Tae Jung Kim is the editor-in-chief, and Ji Sung Lee, Soo-Hyun Park, and Sang-Bae Ko are editorial board members of the journal. However, they were not involved in the peer reviewer selection, evaluation, or decision-making process for this article. No other potential conflicts of interest relevant to this article have been reported.
Acknowledgments
This study was supported by the Seoul National University Hospital (No. 0320210030).
Author contributions
Conceptualization: TJK, SBK. Methodology: TJK, JSL, SBK. Software: TJK, JSL. Supervision: SBK. Validation: SHP. Formal analysis: TJK, JSL. Investigation: TJK, SHP. Resources: TJK, SBK. Data curation: TJK. Visualization: TJK. Project administration: TJK, SBK. Funding acquisition: SBK. Writing–original draft: TJK. Writing–review & editing: TJK, SBK.
Supplementary materialsSupplementary materials can be found via https://doi.org/10.18700/jnc.230030.
Supplementary Table 1.Changes in the pupillometer parameters over 24 hours in acute stroke patients treated with dexmedetomidine (n=5) Fig. 1.Variations in the pupillometer parameters over 24 hours: (A) maximum pupil size, (B) percentage of constriction (%CH), (C) latency (LAT), (D) constriction velocity (CV), (E) maximum constriction velocity (MCV), (F) dilation velocity (DV), (G) neurological pupil index (NPi). Quantitative pupillometry was performed every 4 hours using the NPi-100 pupillometer. Significant diurnal variations are observed in the maximum pupil size, %CH, CV, MCV, and DV during the 24-hour period. The pupillometer parameters, including maximum pupil size, %CH, CV, MCV, and DV show a gradual increase after 20:00 (baseline); the values recorded at 04:00 AM are the highest, whereas those recorded at 20:00 are the lowest. P-value in right (Rt) and left (Lt): P for linear trend. *P<0.05. 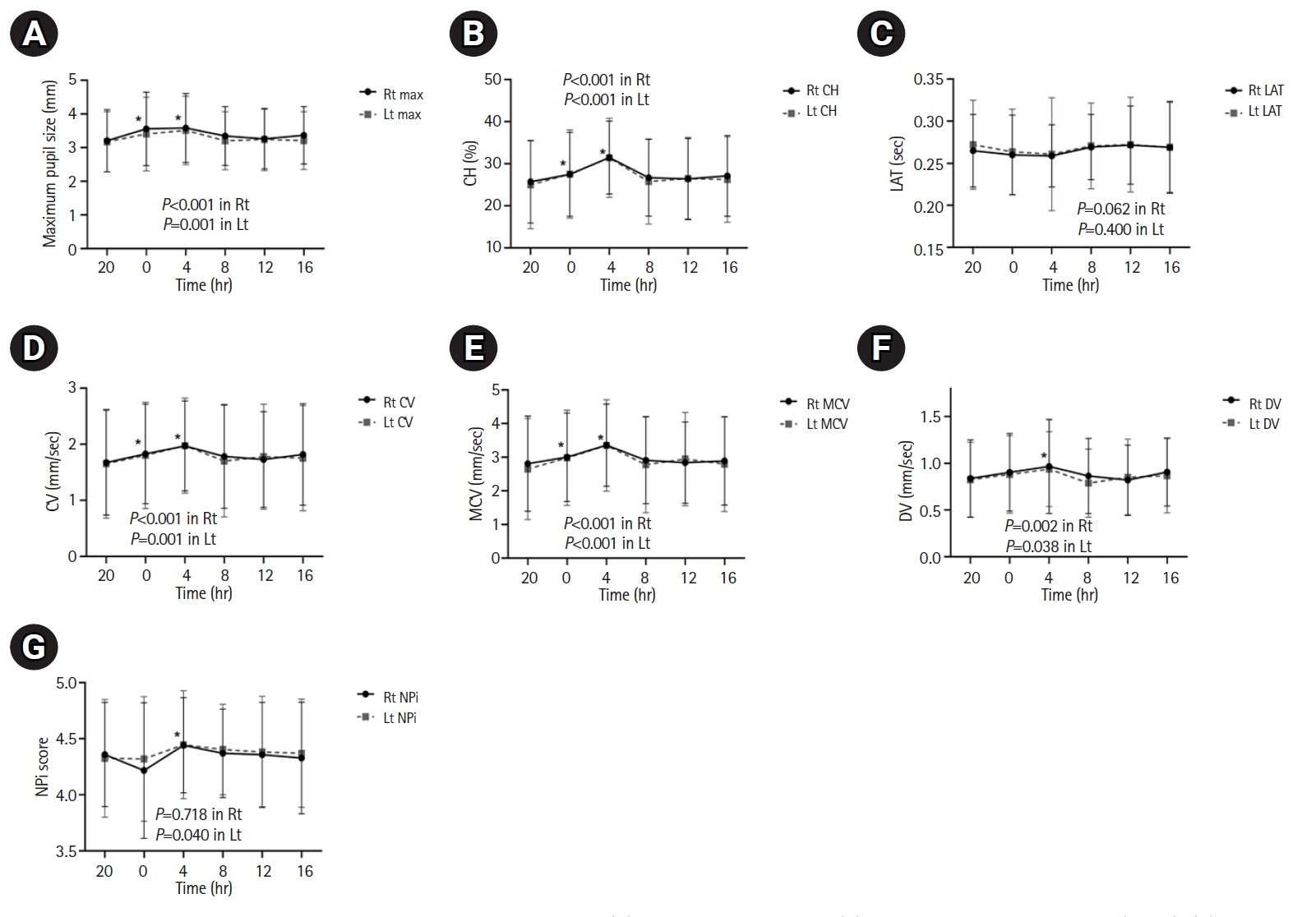
Table 1.Baseline characteristics of the patients Table 2.Pupillometer parameters during the 24-hour monitoring period according to the lesion side Table 3.Change in the pupillometer parameters of acute stroke patients during 24 hours Values are presented as mean±standard deviation. ref, reference; CH, constriction; LAT, latency; CV, constriction velocity; MCV, maximum constriction velocity; DV, dilation velocity; NPi, neurological pupil index. All P-values are calculated using a linear mixed-effect model with a random intercept model for repeated measures analysis. a)P-value for mean difference between 20:00 (baseline) time and each time point in 24 hours. REFERENCES1. Lussier BL, Olson DM, Aiyagari V. Automated pupillometry in neurocritical care: research and practice. Curr Neurol Neurosci Rep 2019;19:71.
2. Zhao W, Stutzman S, DaiWai O, Saju C, Wilson M, Aiyagari V. Inter-device reliability of the NPi-100 pupillometer. J Clin Neurosci 2016;33:79-82.
4. Kim TJ. Quantitative assessments of pupillary light reflexes in neurocritically ill patients. J Neurocrit Care 2022;15:79-87.
5. Kim TJ, Park SH, Jeong HB, Ha EJ, Cho WS, Kang HS, et al. Neurological pupil index as an indicator of neurological worsening in large hemispheric strokes. Neurocrit Care 2020;33:575-81.
6. Chen JW, Gombart ZJ, Rogers S, Gardiner SK, Cecil S, Bullock RM. Pupillary reactivity as an early indicator of increased intracranial pressure: the introduction of the Neurological Pupil index. Surg Neurol Int 2011;2:82.
7. Oddo M, Sandroni C, Citerio G, Miroz JP, Horn J, Rundgren M, et al. Quantitative versus standard pupillary light reflex for early prognostication in comatose cardiac arrest patients: an international prospective multicenter double-blinded study. Intensive Care Med 2018;44:2102-11.
8. Daguet I, Bouhassira D, Gronfier C. Baseline pupil diameter is not a reliable biomarker of subjective sleepiness. Front Neurol 2019;10:108.
9. Wilson MH, Edsell M, Imray C, Wright A; Birmingham Medical Research Expeditionary Society. Changes in pupil dynamics at high altitude: an observational study using a handheld pupillometer. High Alt Med Biol 2008;9:319-25.
10. Münch M, Léon L, Crippa SV, Kawasaki A. Circadian and wake-dependent effects on the pupil light reflex in response to narrow-bandwidth light pulses. Invest Ophthalmol Vis Sci 2012;53:4546-55.
11. Wilhelm B, Giedke H, Lüdtke H, Bittner E, Hofmann A, Wilhelm H. Daytime variations in central nervous system activation measured by a pupillographic sleepiness test. J Sleep Res 2001;10:1-7.
12. Eggert T, Sauter C, Popp R, Zeitlhofer J, Danker-Hopfe H; “Vigilance” of the German Society for Sleep Research and Sleep Medicine (DGSM). The pupillographic sleepiness test in adults: effect of age, gender, and time of day on pupillometric variables. Am J Hum Biol 2012;24:820-8.
14. Couret D, Boumaza D, Grisotto C, Triglia T, Pellegrini L, Ocquidant P, et al. Reliability of standard pupillometry practice in neurocritical care: an observational, double-blinded study. Crit Care 2016;20:99.
15. Lee MH, Mitra B, Pui JK, Fitzgerald M. The use and uptake of pupillometers in the intensive care unit. Aust Crit Care 2018;31:199-203.
16. Lussier BL, Stutzman SE, Atem F, Venkatachalam AM, Perera AC, Barnes A, et al. Distributions and reference ranges for automated pupillometer values in neurocritical care patients. J Neurosci Nurs 2019;51:335-40.
17. Payne WN, Blair K, Barrett MJ. Anisocoria [Internet]. StatPearls Publishing; 2023 [cited 2023 Oct 20]. Available from: https://pubmed.ncbi.nlm.nih.gov/29261943/.
18. Biaggioni I. Circadian clocks, autonomic rhythms, and blood pressure dipping. Hypertension 2008;52:797-8.
19. Loving RT, Kripke DF, Glazner LK. Circadian rhythms in the human pupil and eyelid. Am J Physiol 1996;271(2 Pt 2):R320-4.
20. Wilhelm H, Lüdtke H, Wilhelm B. Pupillographic sleepiness testing in hypersomniacs and normals. Graefes Arch Clin Exp Ophthalmol 1998;236:725-9.
21. Van Egroo M, Gaggioni G, Cespedes-Ortiz C, Ly JQ, Vandewalle G. Steady-state pupil size varies with circadian phase and sleep homeostasis in healthy young men. Clocks Sleep 2019;1:240-58.
22. Jobanputra AM, Scharf MT, Androulakis IP, Sunderram J. Circadian disruption in critical illness. Front Neurol 2020;11:820.
24. Lusczek ER, Knauert MP. Light levels in ICU patient rooms: dimming of daytime light in occupied rooms. J Patient Exp 2021;8:23743735211033104.
|
|
||||||||||||||||||||||||||||||||||||