A 54-year-old female patient presented to the emergency room with vomiting and convulsions, which subsided after the administration of 4 mg of intravenous (IV) lorazepam. The patient was previously diagnosed with neuronal intranuclear inclusion disease (NIID) at another tertiary hospital. The patient was stuporous and had a fever (39.2 ┬░C) and elevated blood pressure (180/90 mm Hg).
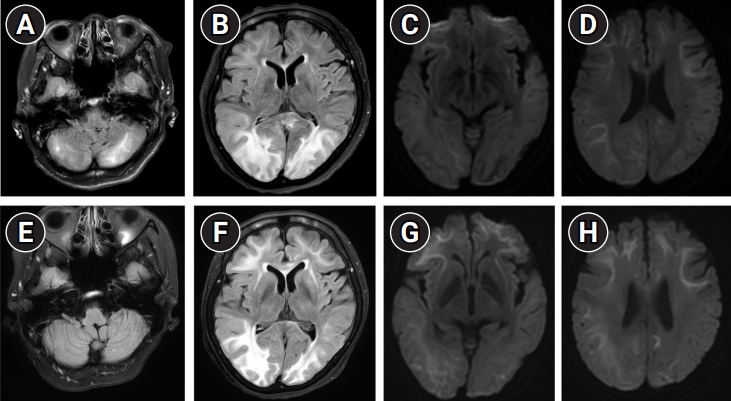
Brain magnetic resonance imaging (MRI) showed high signal intensity in the bilateral parietooccipital lobe and cerebellum on fluid-attenuated inversion recovery (FLAIR), which was suggestive of posterior reversible encephalopathy syndrome (PRES) (Fig. 1A and B) [1,2]. Additionally, MRI revealed bilateral diffusion restriction in the corticomedullary junction on diffusion-weighted imaging (DWI), in accordance with NIID (Fig. 1C and D) [3,4].
Her blood pressure was meticulously adjusted using IV nicardipine [2]. The patient slowly improved and experienced drowsiness. Follow-up brain MRI revealed less prominent FLAIR high signal intensity, which implied improved PRES (Fig. 1E and F). However, the MRI findings of NIID were aggravated, and lesions were more prominent in the bilateral frontotemporal lobes (Fig. 1G and H). At discharge, the patient was alert, and her cognitive impairment and apraxia persisted [4].
Neurologists should always consider the possibility of other conditions, such as PRES, when managing patients with NIID with drowsy mental status and excessively high blood pressure. The highly variable symptoms of NIID might confuse physicians [3].